Drug Overdose Prevention
Related Topics
Determinants of Health: Substance Use
Health starts where people live, learn, work, and play. Conditions of life are connected to healthy outcomes, especially when it comes to the treatment of substance use, chronic pain, mental health, and trauma.
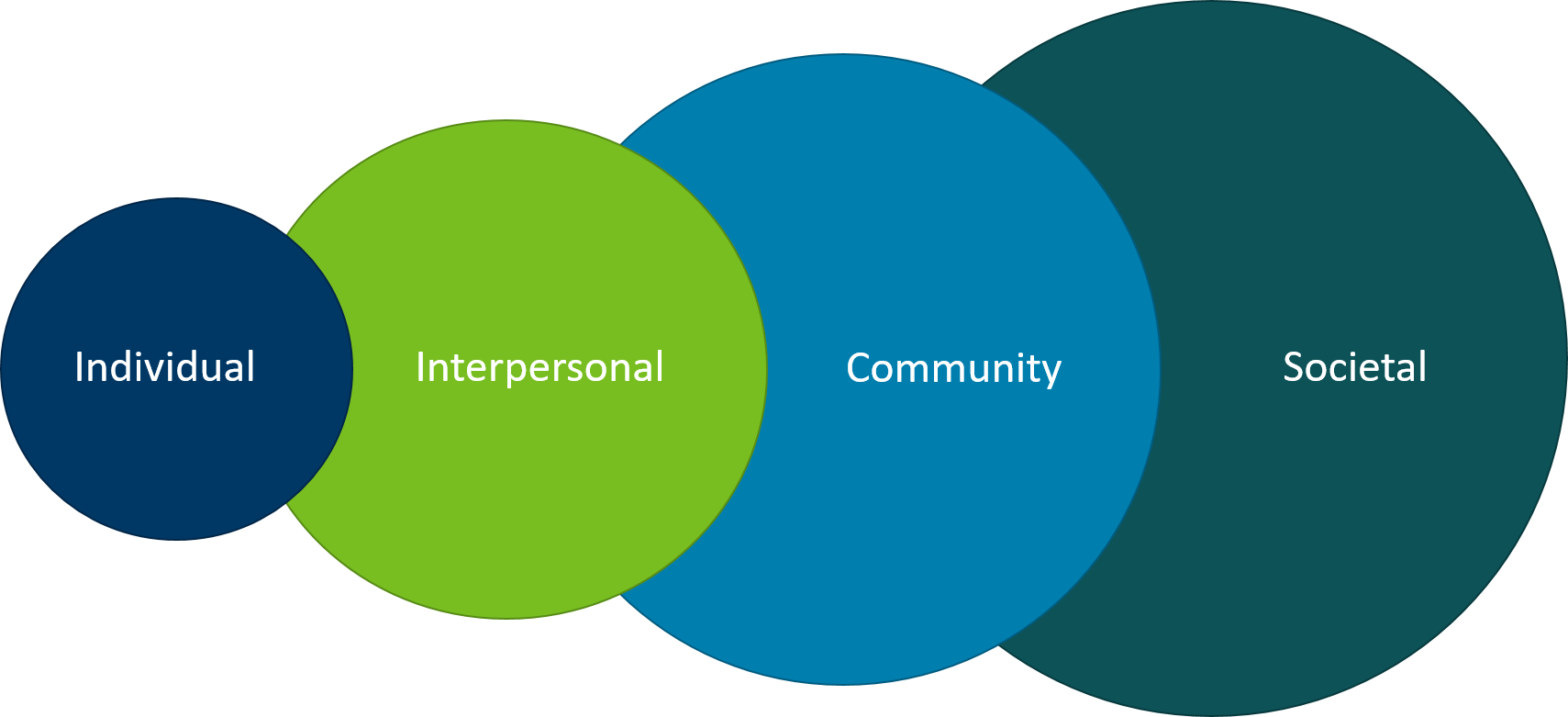
Figure 1: Social-Ecological Model of Substance Use and Overdose Prevention
Determinants of health are the conditions within a home, family, school, and community that can impact a person’s ability to be healthy. Determinants of health include the physical characteristics of the neighborhood a person lives in, access to healthy food, safe housing, quality education, and economic well-being.
Determinants of health are often mapped using a social-ecological model (SEM) that includes multiple levels of the physical and social environments that interact and overlap to impact health. These levels are:
- Individual
- Interpersonal (friends, family, and social groups)
- Community
- Societal
An SEM can be helpful to understand some of the root causes of health disparities. Of important note, no one factor in any level leads a person to use or misuse substances.
Examples of factors at the various levels of an SEM that might influence a person's substance use include:
- Individual:
- Physical and mental health
- Trauma and resiliency
- Social emotional learning and skills
- Perception of risk
- Knowledge of public health and harm reduction
- Withdrawal symptom management
- Interpersonal
- Access to opioids
- Attitudes and opinions towards substance use and pain management
- Acceptance of medication assisted treatment (MAT)
- Substance use identification and prevention education
- Access to peer support and family support
- Naloxone education and carrying
- Family history of substance use
- Community
- Access to culturally-specific providers, peer networks, and behavioral health services
- Prescriber's perception of risk and prescribing practices
- Drug disposal facilities
- Access to MAT
- Access to naloxone and naloxone training
- Public health and harm reduction programming
- Societal
- Stigma towards people who use drugs
- Legislation that supports syringe service programs, MAT, and expansion of behavioral health services
- Polices that promote racial and health equity
- Economic wellbeing and housing stability
- Health insurance coverage for mental health and substance use treatment
- Naloxone protocol for pharmacies
- Impacts of justice involvement on economic and social advancement
Substance use and overdose prevention programming can focus on a single level of the SEM, but interventions that work across multiple levels are more likely to be successful in preventing substance use and overdose. When discussing the determinants of health, it is common to use the terms “upstream” and “downstream” to refer to the levels of an SEM. Upstream refers to policy changes and large-scale prevention efforts, such as by a big hospital system, that have the potential to impact an entire community by addressing determinants of health directly. Downstream refers to treatment and programs that are focused on individual behaviors and health outcomes rather than a larger group of people.
Using the social-ecological model of substance use and overdose prevention (Figure 1), we can trace how a societal change can influence an individual’s health. At the societal level, legislation passed at the state level that supports expanding medication-assisted treatment (MAT) can have a positive impact on a community’s access to MAT as more providers and clinics are able to offer MAT. This policy change would be an upstream intervention. If MAT becomes more accessible in a community, it is possible that people living in that community will learn more about MAT and accept MAT as a type of treatment that people who use drugs can benefit from. If there is greater acceptance of MAT at the interpersonal level, a person using drugs might feel more comfortable using MAT and benefit from a reduction in stigma surrounding this type of treatment. This behavior change would be a downstream outcome.
Preventing substance use and overdose requires a combination of upstream and downstream interventions. To learn more about the types of substance use and overdose prevention, please review the Promising Overdose Prevention Practices.
Health Inequities and Determinants of Health
The negative or positive impact of determinants of health can accumulate over a lifetime, alter a person’s life course, and be passed down to future generations. According to the World Health Organization, about 75% of health inequalities, or differences in outcomes, could be considered unfair and potentially avoidable, and as a result are labeled health inequities. Health inequities are differences in outcomes that are avoidable, unfair, or unjust. In the 2014 MDH Health Equity Report (PDF), structural racism is cited as the main source of health inequities. Structural racism is when decisions are made on a system-wide level that benefit whites and create chronic adverse outcomes for people of color and Indigenous people.
Structural racism has been linked to an increased risk of substance use and overdose. In Minnesota, structural racism has prevented communities of color (particularly Black and Indigenous Minnesotans) from having equal access to the resources needed to be healthy. Poverty, adverse childhood experiences, intergenerational trauma, and intergenerational substance use are all determinants of health influenced by structural racism. The health inequities experienced by communities of color, as a result of determinants of health and structural racism, result in overdose death disparities for communities of color. To learn more about how communities of color in Minnesota are impacted by overdose, please review the Differences in Rates of Drug Overdose Deaths by Race (PDF) report published by MDH.
Another determinant of health closely linked to an increased risk of mental health issues and substance use is adverse childhood experiences (ACEs). ACEs are potentially traumatic events that occur during childhood. ACEs include experiencing or witnessing violence, abuse, or neglect, having a family member attempt or die by suicide, and living in a household with someone that has substance misuse or mental health problems. ACEs do not impact all Minnesotans equally. Minnesotans of color are more likely to have multiple ACEs than white Minnesotans.
The social-ecological model of substance uses, and overdose prevention provides some examples of changes that can be made to improve access to substance use treatment, but it is important that all changes also consider how to reduce the impact of structural racism and ACEs. Prevention services that are culturally specific and trauma-informed can help to reduce health inequities and improve access to appropriate treatment for all Minnesotans.
Resources
- Centers for Disease Control and Prevention: The Social Ecological Model
- Minnesota Department of Health: Adverse childhood experiences in Minnesota (PDF)
Please visit the Opioid Dashboard for more information on opioid overdose death, nonfatal overdose, use, misuse, substance use disorder, prescribing practices, supply, diversion, harm reduction, co-occurring conditions, and social determinants of health.