Annual Summary of Disease Activity:
Disease Control Newsletter (DCN)
Related Topics
Contact Info
Tuberculosis, 2007
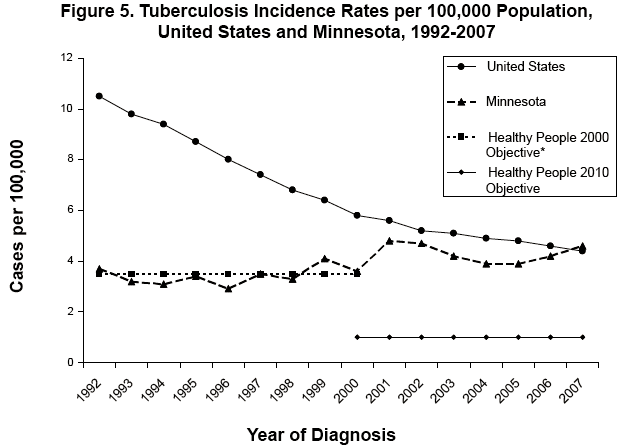
While the number of cases of tuberculosis (TB) disease reported nationally has decreased each year since 1993, the incidence of TB in Minnesota increased throughout much of the 1990s and peaked at 239 TB cases (4.8 cases per 100,000 population) in 2001. After 3 consecutive years (2002-2004) of decreasing incidence followed by a plateau at 199 cases in 2005, the number of reported TB cases in Minnesota has steadily increased. A 9% increase in 2006 resulted in 217 cases, and a 10% increase in 2007 resulted in 238 cases (one case short of the 2001 peak). The increase in cases observed in 2006 primarily was due to a 62% increase in the number of U.S.-born cases, whereas the number of foreign-born cases counted in 2006 was essentially the same as the prior year. In 2007, the increase in cases was due to a 16% increase in the number of foreign-born cases (from 175 to 203), while the number of U.S.-born cases decreased by 17% (from 42 to 35). The 238 cases counted in 2007 represent an incidence rate of 4.6 cases per 100,000 population. The statewide incidence is slightly above that of the national rate (4.4 cases per 100,000 population in 2007); it also exceeds the U.S. Healthy People 2010 objective of 1.0 case per 100,000 population (Figure 5).
The most distinguishing characteristic of the epidemiology of TB disease in Minnesota continues to be the large proportion of TB cases reported among foreign-born persons. During the past decade, the percentage of foreign-born persons among TB cases reported in Minnesota increased from 71% in 1998, to 87% in 2005. In 2007, 85% of TB cases in Minnesota were foreign-born, which is consistent with the average percentage of foreign-born cases (83%) reported from 2003 through 2007. In contrast, 59% of TB cases reported nationwide in 2007 were foreign-born.
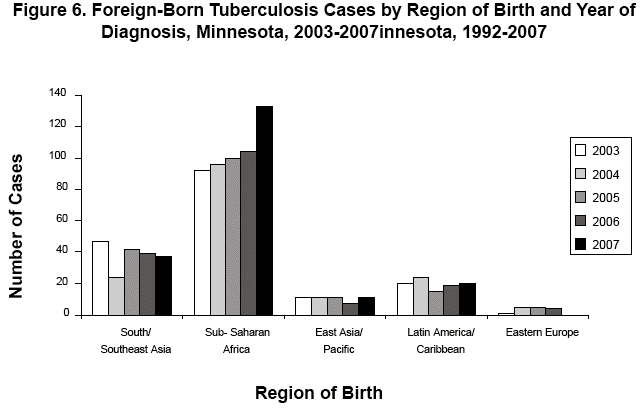
The 203 foreign-born 2007 TB case-patients represent 27 different countries of birth. The most common region of birth among foreign-born TB cases reported in 2007 was sub-Saharan Africa (66%), followed by South/Southeast Asia (18%) (Figure 6). The ethnic diversity among these foreign-born TB cases reflects the unique and constantly changing demographics of immigrant and other foreign-born populations arriving in Minnesota. This diversity also poses significant challenges in providing culturally and linguistically appropriate TB prevention and control services for populations most affected by and at risk for TB in Minnesota.
Nearly one-fourth (24%) of the foreign-born TB case-patients reported in 2007 were diagnosed within 12 months after arriving in the United States. These cases likely represent persons who acquired TB infection outside the United States and began progressing to active TB disease prior to immigrating. Persons 15 years of age or older who arrive in the United States as immigrants or refugees receive a pre-immigration medical examination overseas that includes screening for pulmonary TB disease. Of 34 TB case-patients 15 years of age or older who were diagnosed in Minnesota during 2007 within 12 months of arriving in the United States and who arrived as immigrants or refugees, only nine (26%) had any TB-related condition noted in their pre-immigration medical exam results. These findings highlight the need for clinicians to have a high index of suspicion for TB among newly arrived foreign-born persons, regardless of the results of medical exams performed overseas. More than half (62%) of foreign-born TB case-patients reported in Minnesota during 2007 were diagnosed 2 or more years after arriving in the United States. These data suggest that at least half of foreign-born TB cases reported in Minnesota may be preventable by focusing on thorough domestic screening, evaluation, and treatment of latent TB infection among recently arrived refugees, immigrants, and other foreign-born persons.
The majority (68%) of foreign-born TB case-patients reported in Minnesota in 2007 were 15 to 44 years of age, whereas only 20% of U.S.-born TB cases occurred among persons in this age category. In contrast, 54% of U.S.-born TB case-patients were 45 years of age or older. The proportion of pediatric patients less than 5 years of age was considerably larger among U.S.-born TB cases than among foreign-born cases (11% versus 0%, respectively), although nearly all of these U.S.-born case-patients were children born in the U.S. to foreign-born parents. These first-generation U.S.-born children appear to experience an increased risk of TB disease that more closely resembles that of foreign-born persons. Presumably, these children may be exposed to TB as a result of travel to their parents’ country of origin and/or visiting or recently arrived family members who may be at increased risk for TB acquired overseas.
The majority (81%) of TB cases in 2007 in Minnesota were identified as a result of presenting for medical care. Other methods of case identification during this time period included TB contact investigations (6%), domestic refugee health examinations (6%), and follow-up evaluations following abnormal findings on pre-immigration exams performed overseas (3%). The remaining 4% of TB cases were identified through a variety of other means.
Aside from foreign-born persons, other high-risk population groups comprise much smaller proportions of the TB cases reported in Minnesota. Among cases reported in 2007, persons with certain medical conditions (excluding HIV infection) that increase the risk for progression from latent TB infection to active TB disease (e.g., silicosis, diabetes, prolonged corticosteroid therapy or other immunosuppressive therapy, end stage renal disease, etc.) were the most common of these other high-risk population groups, representing 16% of the cases. Substance abuse (including alcohol abuse and/or illicit drug use) was the second most common of these other risk factors, with approximately 7% of TB case-patients having a history of substance abuse during the 12 months prior to their TB diagnosis. Twelve (5%) of the 238 TB case-patients reported in Minnesota during 2007 were infected with HIV; all 12 of those HIV-infected TB case-patients were foreign-born, including four persons born in Mexico, two persons each from Ethiopia, Kenya, Liberia, and one person each from Cameroon and Sudan. The percentage of TB case-patients in Minnesota with HIV co-infection remains less than that among all TB cases reported nationwide. Other risk groups such as homeless persons, correctional facility inmates, and residents of nursing homes each represented only 1-3% of TB cases reported in Minnesota during 2007.
Twenty-seven (31%) of the state’s 87 counties reported at least one case of TB disease in 2007, with the majority (79%) of cases occurring in the metropolitan area, particularly in Hennepin (48%) and Ramsey (20%) Counties, both of which have public TB clinics. Eleven percent of TB cases occurred in the five suburban metropolitan counties (i.e., Anoka, Dakota, Carver, Scott, and Washington). Olmsted County, which maintains a public TB clinic staffed jointly by the Olmsted County Health Department and Mayo Clinic, represented 8% of cases reported statewide in 2007. The remaining 13% of cases occurred in primarily rural areas of Greater Minnesota. MDH calculates county-specific annual TB incidence rates for Hennepin, Ramsey, and Olmsted counties, as well as for the five-county suburban metropolitan area and collectively for the remaining 79 counties in Greater Minnesota. In 2007, the highest TB incidence rate (14.3 cases per 100,000) was reported in Olmsted County, followed by Hennepin and Ramsey counties, respectively. The TB incidence rate in Hennepin County increased from 8.4 cases per 100,000 in 2006 to 10.0 cases per 100,000 in 2007, while the TB incidence rate in Ramsey County increased from 8.5 cases per 100,000 in 2006 to 9.4 cases per 100,000 in 2007. In 2007, the incidence rates in both the five-county suburban metropolitan area (2.2 cases per 100,000) and Greater Minnesota (1.4 cases per 100,000) were considerably lower than that in the state overall.
Drug-resistant TB is a critical concern in the prevention and control of TB in Minnesota, as well as nationally and globally. The prevalence of drug-resistant TB in Minnesota, particularly resistance to isoniazid (INH) and multi-drug resistance, exceeds comparable national figures. In 2007, 22 (13%) of 176 culture-confirmed TB cases were resistant to at least one first-line anti-TB drug (i.e., INH, rifampin, pyrazinamide, or ethambutol). In particular, 17 (10%) cases were resistant to INH, and three (2%) cases were multidrug-resistant (i.e., resistant to at least INH and rifampin). These data reflect the prevalence of MDR-TB in Minnesota during the past 5 years, which averaged approximately 2% of cases annually. Drug resistance is more common among foreign-born TB cases than it is among U.S.-born cases in Minnesota. Of particular concern, six (32%) of 19 MDR-TB cases reported from 2003 through 2007 were resistant to all four first-line drugs. These six pan-resistant MDR-TB case-patients represented six different countries of birth (one each from China, Ethiopia, Laos, Thailand, Somalia, and the United States). The U.S.-born pan-resistant patient was a young child infected by a foreign-born family member. One of the MDR-TB cases (2006) also met the current World Health Organization definition of extensively drug-resistant (XDR) TB.
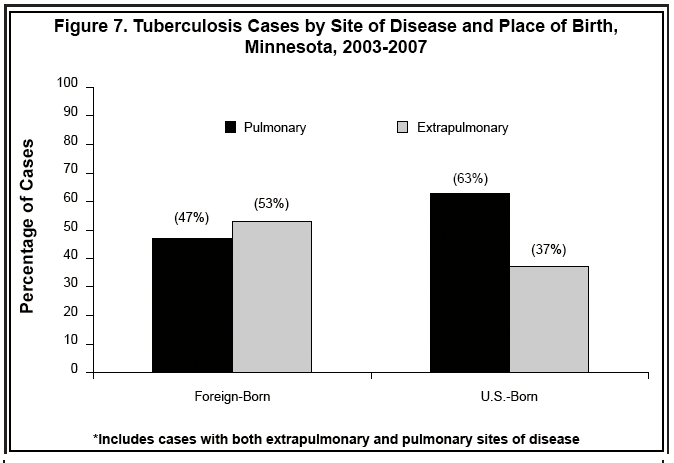
Another clinical characteristic of significance among TB cases in Minnesota is the preponderance of extrapulmonary disease among foreign-born TB patients. Just over half (53%) of foreign-born TB case-patients counted from 2003 through 2007 had an extrapulmonary site of disease; in contrast, only 37% of U.S.-born TB case-patients had extrapulmonary TB (). The most common extrapulmonary sites of TB disease in Minnesota are lymphatic, pleural, peritoneal, bone/joint, and meningeal. The unusually high incidence of extrapulmonary TB disease in Minnesota exemplifies the need for clinicians to be aware of the epidemiology of TB in Minnesota and to have a high index of suspicion for TB, particularly among foreign-born patients and even when the patient does not present with a cough or other common symptoms of pulmonary TB.
The epidemiology of TB in Minnesota highlights the need to support global TB elimination strategies, as well as local TB prevention and control activities targeted to foreign-born persons. TB in Minnesota occurs primarily, although not exclusively, among foreign-born persons, with TB case-patients representing many countries of origin and varied cultural backgrounds. The prevalence of drug-resistant TB in Minnesota is high compared to that of the national rate, and extrapulmonary sites of disease are common, especially among foreign-born cases. The proportion of TB cases occurring in persons under 5 years of age in Minnesota exceeds the comparable figure nationally, with many of these children being born to foreign-born parents. These trends suggest that the incidence of TB in Minnesota is not likely to decrease in the foreseeable future.
- For up to date information see>> Tuberculosis (TB)
- Full issue>> Annual Summary of Communicable Diseases Reported to the Minnesota Department of Health, 2007