Annual Summary of Disease Activity:
Disease Control Newsletter (DCN)
Related Topics
Contact Info
Sexually Transmitted Diseases, 2008
STD Diseases on this page:
Chlamydia
Gonorrhea
Syphilis
Chancroid
Active surveillance for gonorrhea and chlamydia involves cross-checking laboratory-reported cases against cases reported by clinicians. Although both laboratories and clinical facilities are required to report STDs independently of each other, an episode of STD is not considered a case for surveillance purposes until a corresponding case report is submitted by a clinical facility. Case reports contain demographic and clinical information that is not available from laboratory reports. When a laboratory report is received but no corresponding case report is received within 45 days, MDH mails a reminder letter and case report form to the corresponding clinical facility. Active surveillance for syphilis involves immediate follow-up with the clinician upon receipt of a positive laboratory report. Cases of chancroid are monitored through a mostly passive surveillance system. Herpes simplex virus and human papillomavirus infections are not reportable.
Although overall incidence rates for STDs in Minnesota are lower than those in many other areas of the United States, certain population subgroups in Minnesota have very high STD rates. Specifically, STDs disproportionately affect adolescents, young adults, and persons of color.
Chlamydia
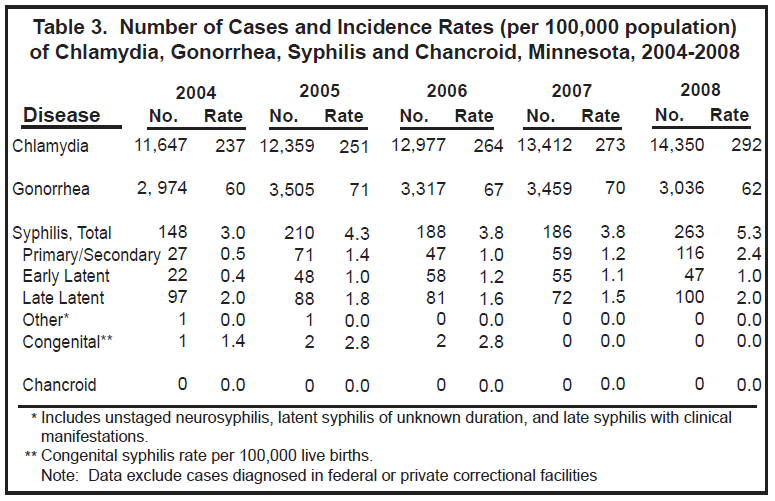
Chlamydia trachomatis infection is the most commonly reported infectious disease in Minnesota. In 2008, 14,350 chlamydia cases (292 per 100,000 population) were reported, representing a 7% increase from 2007 (Table 3).
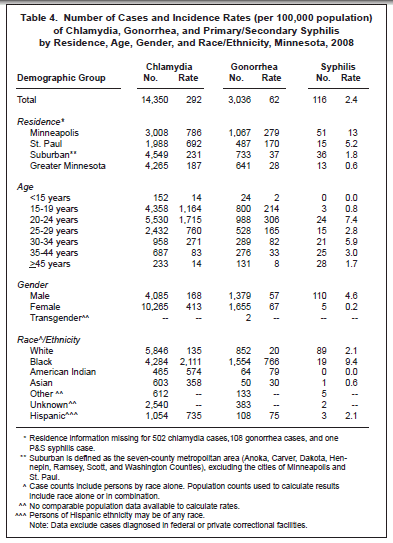
Adolescents and young adults are at highest risk for acquiring chlamydial infection (Table 4). The chlamydia rate is highest among 20 to 24-year-olds (1,715 per 100,000), with the next highest rate among 15 to 19-year-olds (1,164 per 100,000). The incidence of chlamydia among adults 25 to 29 years of age (760 per 100,000) is considerably lower but has increased in recent years. The chlamydia rate among females (413 per 100,000) is more than twice the rate among males (168 per 100,000), a difference most likely due to more frequent screening among women.
The incidence of chlamydia infection is highest in communities of color (Table 4). The rate among blacks (2,111 per 100,000) is 16 times higher than the rate among whites (135 per 100,000). Although blacks comprise approximately 4% of Minnesota’s population, they account for 30% of reported chlamydia cases. Rates among Asian/Pacific Islanders (358 per 100,000), American Indians (574 per 100,000), and Hispanics (735 per 100,000) are three to six times higher than the rate among whites.
Chlamydia infections occur throughout the state, with the highest reported rates in Minneapolis (786 per 100,000) and St. Paul (692 per 100,000). However, in 2008 the greatest increases for chlamydia were seen in the suburbs and Greater Minnesota with increases of 9% and 10%, respectively.
Gonorrhea
Gonorrhea, caused by Neisseria gonorrhoeae, is the second most commonly reported STD in Minnesota. In 2008, 3,036 cases (62 per 100,000 population) were reported, representing a 12% decrease from 2007 (Table 3).
Adolescents and young adults are at greatest risk for gonorrhea (Table 4), with incidence rates of 214 per 100,000 among 15 to 19-year-olds, 306 per 100,000 among 20 to 24-year olds, and 165 per 100,000 among 25 to 29-year-olds. Gonorrhea rates for males (57 per 100,000) and females (67 per 100,000) are comparable. Communities of color are disproportionately affected by gonorrhea, with one half of cases reported among blacks. The incidence of gonorrhea among blacks (766 per 100,000) is 38 times higher than the rate among whites (20 per 100,000). Rates among Asian/Pacific Islanders (30 per 100,000), American Indians (79 per 100,000), and Hispanics (75 per 100,000) are two to four times higher than among whites.
Gonorrhea rates are highest in the cities of Minneapolis and St. Paul (Table 4). The incidence in Minneapolis (279 per 100,000) is 60% higher than the rate in St. Paul (170 per 100,000), nearly eight times higher than the rate in the suburban metropolitan area (37 per 100,000), and 10 times higher than the rate in Greater Minnesota (28 per 100,000). However, the rate in Greater Minnesota is growing rapidly, increasing 14% in 2008 while the rest of the state is seeing large decreases.
Quinolone-resistant N. gonorrhoeae
The prevalence of quinolone-resistant N. gonorrhoeae (QRNG) has increased approximately four-fold from 1.5% in 2002 to 6.3% in 2008. Of special concern is the high prevalence among men who have sex with men (MSM), which increased sharply from 0% in 2002, to 8.9% in 2003, and to 27% in 2004. Since then the prevalence in this population has remained high (15% in 2008). In 2007, QRNG prevalence also reached a critical level in heterosexuals (4.5%), prompting the MDH to recommend non-quinolone therapy for that population as well. As a result, fluoroquinolones (eg, ciprofloxacin) are no longer recommended for treating gonorrhea in Minnesota.
Syphilis
Surveillance data for primary and secondary syphilis are used to monitor morbidity trends because they represent recently acquired infections. Data for early syphilis (which includes primary, secondary, and early latent stages of disease) are used in outbreak investigations because they represent infections acquired within the past 12 months and signify opportunities for disease prevention.
Primary and Secondary Syphilis
The incidence of primary/secondary syphilis in Minnesota is lower than that of chlamydia or gonorrhea (Table 3), but has remained elevated since an outbreak was observed in 2002 among men who have sex with men (MSM). This sustained outbreak reached a new level in 2008, with 116 cases of primary/secondary syphilis (2.4 per 100,000 population) being reported compared to 59 (1.2 per 100,000) cases in 2007.
Early Syphilis
In 2008, the number of early syphilis cases increased by 43%, with 163 cases occurring compared to 114 cases in 2007. The incidence remains highly concentrated among MSM. Of the early syphilis cases in 2008, 158 (97%) occurred among men; 140 (89%) of these men reported having sex with other men; 46% of the MSM diagnosed with early syphilis were co-infected with HIV.
Congenital Syphilis
No cases of congenital syphilis were reported in Minnesota in 2008 (Table 3).
Chancroid
Chancroid continues to be very rare in Minnesota. No cases were reported in 2008.
- For up to date information see>> Sexually Transmitted Diseases (STDs)
- Full issue>> Annual Summary of Communicable Diseases Reported to the Minnesota Department of Health, 2008