Annual Summary of Disease Activity:
Disease Control Newsletter (DCN)
Related Topics
Contact Info
Influenza, 2009
In April, 2009, novel A H1N1 emerged as a new influenza virus starting the first influenza pandemic in over 30 years.
Hospitalized Cases
Surveillance for pediatric (<18 years of age) laboratory-confirmed hospitalized cases of influenza was established during the 2003-2004 influenza season. During the 2006-2007 season surveillance was expanded to include adults. During the novel H1N1 pandemic period (April 2009-April 2010), MDH requested that clinicians collect a throat or nasopharyngeal swab or other specimen from all patients admitted to a hospital with suspect influenza and submit the specimen to the PHL for influenza testing.
During the pandemic period there were 1,824 laboratory-confirmed hospitalized cases of H1N1 influenza, 34.9 hospitalizations per 100,000 persons, compared to 5.8 hospitalizations per 100,000 during the 2008-2009 influenza season. Since September 1, 2009, other hospitalized cases of influenza have included 239 that were untypeable influenza A (likely novel H1N1), and 77 that were positive by rapid influenza testing only but these cases could not be further characterized because specimens weren't available for additional testing at the PHL.
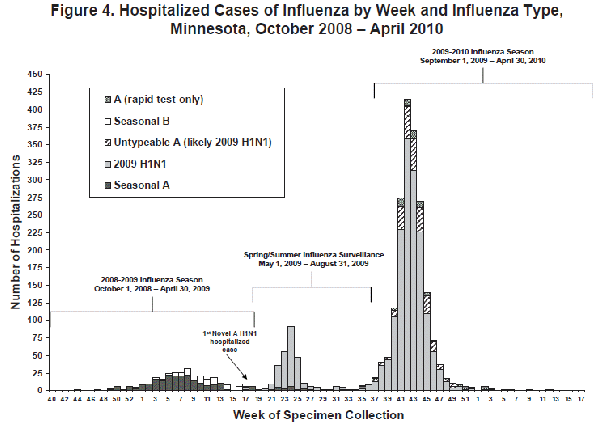
There was a 500% increase in the number of laboratory-confirmed influenza hospitalizations in the pandemic season compared to the 2008-2009 influenza season (Figure 4). Whereas the typical influenza season has peak activity during late December, January, or February, the pandemic period was noted to have two distinct waves, with a peak in cases in late October-November. The pandemic period was also notable for the near complete replacement of seasonal influenza strains with 2009 novel H1N1 influenza.
Among hospitalized 2009 novel H1N1 cases, 44% were <18 years of age, 7% were 18-24 years of age, and 49% were 25 years of age and older. Median age was 24.1 years. Fifty-six percent of cases were residents of the metropolitan area. Six hundred seventy-eight (37%) of 1,824 cases were diagnosed with pneumonia. Three hundred fifty-two (19%) cases required admission into an intensive care unit. Of these, 166 (47%) were placed on mechanical ventilation. Thirty (2%) cases had an invasive bacterial co-infection. Eighty-three percent of adult and 51% of pediatric cases had at least one chronic medical condition that would put them at increased risk for influenza disease.
Deaths
During the pandemic period, MDH increased its efforts to identify deaths related to influenza. All deaths among persons with recent influenza-like illness (ILI) were investigated. Specimens were submitted to MDH and tested by PCR, culture, and serology at the PHL or at the CDC Infectious Diseases Pathology Branch. In addition to investigating deaths reported through hospital surveillance, MDH partnered with medical examiners and hospital pathologists to identify cases. Death certificates were also used to identify any deaths with influenza, "flu," or H1N1 listed as a cause of death and as a means of cross-checking known hospitalized 2009 H1N1 cases.
During the pandemic period, there were 63 novel H1N1 confirmed deaths, 4 influenza A-type unspecified deaths, 2 influenza B deaths, and 3 deaths associated with an influenza syndrome where no testing was performed. The median age was 51 years. Three (4%) deaths were among persons 0-4 years, 6 (9%) 5-18 years, 23 (32%) 19-49 years, 24 (33%) 50-64 years, and 16 (22%) 65 years of age and older. Forty-four percent of cases were from the metropolitan area. Sixty-one (85%) cases had underlying medical conditions, and 57 (79%) had been hospitalized.
Laboratory Data
The Minnesota Laboratory System (MLS) Influenza Surveillance Program is made up of more than 100 clinic- and hospital-based laboratories, voluntarily submitting rapid test data on a weekly basis. Eight of the laboratories report viral culture testing results. Tracking these data assists health care providers with diagnosis of ILI and provides an indicator of the progression of the influenza season as well as prevalence of other respiratory disease pathogens in the community.
Between August 30, 2009 and May 1, 2010, laboratories reported on 44,484 rapid influenza tests; 6,146 (14%) were positive for influenza. Of these, 5,963 (97%) were positive for influenza A, 65 (1%) were positive for influenza B, and 118 (2%) were positive for influenza A/B not differentiated. Percent positive of rapid influenza tests peaked October 18-24, 2009 at 27%. Between August 30, 2009 and May 1, 2010, Minnesota virology laboratories reported data on 10,990 viral cultures, 844 (8%) of which were positive for influenza. Of these, 841 (>99%) were positive for influenza A and 3 (0.4%) were positive for influenza B. Percent positive of influenza cultures peaked during November 1-7, 2009 at 27%.
Between April 2009 and April 2010, 318 (98%) of 324 influenza isolates further characterized in the PHL were subtyped as influenza A 2009 H1N1, 5 (2%) were subtyped as influenza A-type unspecified, and 1 (0.3%) was influenza B/Brisbane-like.
Influenza Sentinel Surveillance
MDH has conducted sentinel surveillance for ILI through outpatient medical providers since 2000 as a way to monitor the impact of influenza. Sentinel provider sites include private practice clinics, public health clinics, urgent care centers, emergency rooms, and college student health centers. In 2009-2010, there were 27 sites in 21 counties. Participating providers report the total number of patient visits each week and number of patient visits for ILI by age group (0-4 years, 5-24 years, 25-64 years, >65 years). Percentage of ILI peaked October 11-17, 2009 at 6.1%. Sentinel providers also submit specimens to the PHL for PCR testing from a subset of patients. From April 2009 to April 2010, the PHL tested 1,414 specimens for influenza by PCR; 453 (32%) were confirmed influenza A 2009 H1N1, 25 (2%) influenza A-type unspecified, 3 (0.2%) seasonal influenza A/(H1), 3 (0.2%) seasonal influenza A/(H3), and 2 were influenza B (0.1%).
ILI Outbreaks (Schools and Long Term Care Facilities)
Between 1988 to 2009, a probable outbreak of ILI in a school was defined as a doubled absence rate with all of the following primary influenza symptoms reported among absent students: rapid onset, fever, illness lasting 3 or more days, and at least one secondary influenza symptom (e.g., myalgia, headache, cough, coryza, sore throat, or chills). A possible ILI outbreak in a school was defined as a doubled absence rate with reported symptoms, including two of the primary influenza symptoms and at least one secondary symptom. Prior to the 2009-2010 influenza season, the number of schools reporting influenza outbreaks ranged from a low of 38 schools in 20 counties in 1996-1997 to 441 schools in 71 counties in 1991-1992.
The definition of ILI outbreaks changed for the 2009-2010 school year. Schools reported when the number of students absent with ILI reached 5% of total enrollment or three or more students with ILI were absent from the same elementary classroom. During the 2009-2010 school year, 1,302 schools in 85 counties reported ILI outbreaks.
An influenza outbreak is suspected in a long-term care facility (LTCF) when three or more residents in a single unit present with a cough and fever or chills during a 48- to 72-hour period. An influenza outbreak is confirmed when at least one resident has a positive culture, PCR, or rapid antigen test for influenza. Four facilities in four counties reported outbreaks from April 2009 – April 2010. Three facilities reported outbreaks in 2008-2009. Surveillance for outbreaks in LTCFs began in the 1988-1989 season. Prior to the 2008-2009 season, the number of long-term care facilities reporting ILI outbreaks has ranged from a low of six in 1990-1991 to a high of 140 in 2004-2005.
- For up to date information see>> Influenza (Flu)
- Full issue>> Annual Summary of Communicable Diseases Reported to the Minnesota Department of Health, 2009