Annual Summary of Disease Activity:
Disease Control Newsletter (DCN)
Related Topics
Contact Info
Tuberculosis, 2017
In 2017, 178 tuberculosis (TB) cases (3.2 per 100,000 population) were reported. This represents a 6% increase in the number of cases compared to 2016, when there were 168 cases. The TB incidence rate in Minnesota has typically been lower than the overall rate in the United States, but Minnesota’s rate in the last couple of years has been higher than the national rate (2.8 per 100,000 in 2017). Despite an increase in the number and rate of new cases in Minnesota over the past few years, the TB case count has decreased 25% since 2007, when 238 cases were reported, and has remained under 200 since 2009. Eight (4%) cases from 2017 have died, 4 of whom died due to TB disease.
There was an increase in the number of TB cases in the youngest and oldest age groups, two groups at higher risk of developing active TB disease. In 2017, 7% of TB cases were <5 years at the time of diagnosis, compared to 4% in 2016. Twenty-two percent of cases were 65 years of age and older, compared to 16% in 2016.
Twenty-two (25%) counties had at least 1 TB case in 2017. The majority (73%) of cases occurred in the metropolitan area, primarily in Hennepin (39%) and Ramsey (21%) Counties. Twenty-two (12%) were from the other 5 metropolitan counties. The remaining 27% of cases were reported from Greater Minnesota, representing a 4% increase from 2016. Among metropolitan area counties, the highest TB incidence rate in 2017 was reported in Ramsey County (7.0 per 100,000), followed by Hennepin County (5.7 per 100,000). The TB incidence rate for all Greater Minnesota counties combined was 1.9 per 100,000.
Most (78%) TB cases were identified as a result of individuals seeking medical care for symptoms of disease. Various targeted public health interventions identified the majority of the remaining 22% of cases. Such case identification methods are high priority core prevention and control activities and include contact investigations (14%), domestic refugee health assessments (1%), and follow- up evaluations of individuals with abnormal findings on pre- immigration exams where infectious TB disease had been ruled out (<1%). An additional 3% were identified through other screening (e.g., other immigration medical exams, employment screening, other targeted testing for TB). Six (3%) cases were diagnosed with active TB disease incidentally while being evaluated for another medical condition.
TB incidence is disproportionately high among racial and ethnic minorities in Minnesota as well as in the United States. In 2017, 7 cases occurred among non-Hispanic whites, a case rate of 0.2 per 100,000. In contrast, among non-Hispanic persons of other races, 95 cases occurred among Africans/blacks (25.8 cases per 100,000), 51 among Asian/Pacific Islanders (17.9 cases per 100,000), and 6 cases among American Indian/Alaska Natives (8.9 cases per 100,000). Nineteen cases were Hispanic persons of any race (6.6 cases per 100,000). The majority of Hispanic (68%), black (84%), and Asian cases (100%) were non-U.S. born.
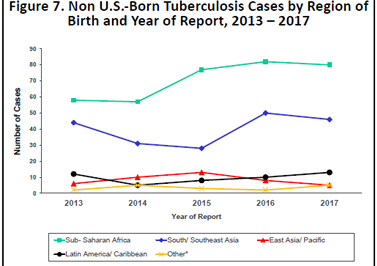
In 2017, the percentage of TB cases in Minnesota occurring in persons born outside the United States was 84%, compared to 70% of TB cases reported nationally. The 149 non- U.S. born TB cases represented 31 different countries of birth; the most common region of birth among these cases was Sub-Saharan Africa (54% of non-U.S. born cases), followed by South/Southeast Asia (31%), Latin America (including the Caribbean) (9%), and East Asia/Pacific (3%). Patients from other regions (North Africa/Middle East, Eastern Europe, and Western Europe) accounted for the remaining 3% of cases (Figure 7).
Individuals in other high risk groups comprised smaller proportions of the cases. Note that patients may fall under more than one risk category. Thirty-one percent occurred in persons with certain medical conditions that increase the risk for progression from latent TB infection (LTBI) to active TB disease (e.g., diabetes, prolonged corticosteroid or other immunosuppressive therapy, end stage renal disease), up from 18% in 2016. The next most common risk factor was substance abuse (including alcohol abuse and/ or injection and non-injection drug use) during the 12 months prior to their TB diagnosis (4%). Four percent of cases were co-infected with HIV, down from 7% in 2016. Four percent also reported being homeless during the 12 months prior to diagnosis, 3% were residents of long-term care facilities, and 1% were in a correctional facility at time of diagnosis.
By site of disease, 54% of cases had pulmonary disease exclusively. Another 13% had both pulmonary and extrapulmonary sites of disease, and 32% had extrapulmonary disease exclusively. Among the 81 patients with an extrapulmonary site of disease, the most common sites were lymphatic (52%), followed by musculoskeletal (21%). Extrapulmonary disease is generally more common among persons born outside the United States. Fifty-two percent of non-U.S. born patients had at least one extrapulmonary site of disease, compared to only 10% of U.S.-born cases.
Of 141 culture-confirmed TB cases with drug susceptibility results available, 32 (23%) were resistant to at least one first-line anti-TB drug (i.e., isoniazid [INH], rifampin, pyrazinamide, or ethambutol), including 22 (16%) cases resistant to at least INH. There were 9 new cases of multidrug-resistant TB (MDR-TB or resistance to at least INH and rifampin) reported in 2017, compared to 8 MDR-TB cases in 2016. In the 5-year period before that (2011- 2015), there were a total of 5 MDR-TB cases.
- For up to date information see>> Tuberculosis (TB)
- Full issue>> Annual Summary of Communicable Diseases Reported to the Minnesota Department of Health, 2017