Stroke Quality Improvement Awards 2022
The Minnesota Stroke System includes 13 Comprehensive Stroke Centers (CSC), 10 Primary Stroke Centers (PSC), and 92 Acute Stroke Ready Hospitals (ASRH). All hospitals in the Minnesota Stroke System continually strive to improve patient care. This award program aims to recognize and showcase successful quality improvement initiatives throughout the state of Minnesota’s hospital-based stroke programs.
2022 Award Categories
Awards are given to hospital stroke programs in Minnesota that implemented the best quality improvement initiatives in the following categories:
- Continuous Impact: This is an award for starting an initiative that created a meaningful and long-term improvement in the quality of stroke care.
- Operational Excellence: This is an award for an initiative that focused on collaboration between different programs to improve the quality of stroke care.
- Outstanding Achievement: This is an award for an initiative that led to evidence-based positive change in the quality of stroke care.
2022 Continuous Impact Award Recipients
This is an award for starting an initiative that created meaningful and long-term improvement in the quality of stroke care.
Allina Health Faribault Medical Center,
Acute Stroke Ready Hospital
Faribault, Minnesota
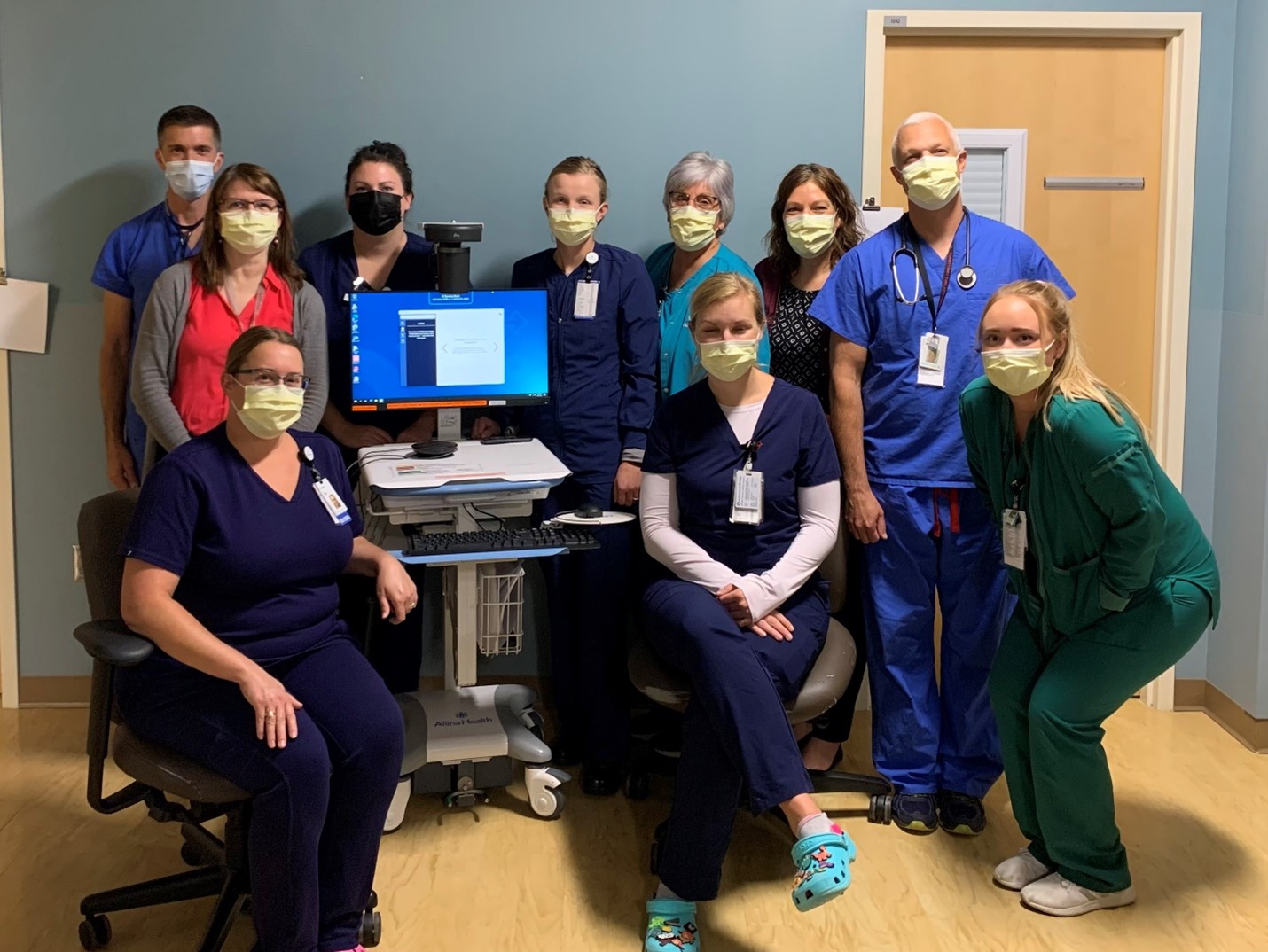
- Opportunity for Improvement: Improve door-to-imaging and door-to-imaging read time to meet the new system goal for door-to-telestroke.
- Action Plan: After reviewing stroke records and workflow, the team identified many areas that could help meet the goal of shortening door-to-imaging times. Assessing and clarifying roles while working together with radiology, EMS, ED registration staff, and nursing staff helped fix multiple issues with the process.
- Results: Met the goal in May of 2022, with over 70% of patients receiving door-to-imaging in under 10 minutes.
Award Qualifications
- Thoughtful, thorough approach to listening to direct patient care staff and addressing their shared issues.
- Strong next steps identified to address health equity in the community they serve.
Mayo Clinic Health System,
Comprehensive Stroke Center: Rochester
Primary Stroke Centers: Eau Claire, La Crosse, and Mankato
Rochester & Mankato, Minnesota; Eau Claire & LaCrosse, Wisconsin
- Opportunity for Improvement: Stroke care across the health system has been standardized, but not the stroke coordinator role. This makes it difficult to succeed. The team set out to improve onboarding, support, collaboration, and mentorship for the new and current primary stroke center coordinators.
- Action Plan: Stroke coordinators from the health system’s primary and comprehensive stroke centers identified main gaps and concerns using the Five Why Tool. After running multiple PDSA cycles, the stroke coordinator team created a standardized stroke coordinator orientation. The program had required learning materials to increase skills and confidence for stroke coordinators. They worked together to create a support system to help prepare for regulatory visits before, during, and after the visit.
- Results: The team met the goal of having a strong system in place to help stroke coordinators succeed in their positions. New stroke coordinators have reported improvement in many areas, including job satisfaction, teamwork, and knowledge. All primary stroke center sites involved had successful re-certifications. All primary stroke center sites involved had onsite support from a fellow stroke coordinator and successful recertification.
Award Qualifications
- Recognized the important role of the stroke coordinator in quality stroke care and the benefits of collaboration.
- Created a lasting impact by setting up other stroke coordinators to succeed in the health system for the future.
2022 Operational Excellence Award Recipients
This is an award for an initiative that focused on collaboration between different programs to improve the quality of stroke care.
Winona Health Services,
Acute Stroke Ready Hospital
Winona, Minnesota

- Opportunity for Improvement: Address many areas of improvement in stroke care while making the change to tenecteplase.
- Action Plan: The team brought together many departments to plan an approach, set priorities, and create a timeline and work plan. They used tools, updates to the electronic health record, different educational opportunities for staff, and collaborated with a primary stroke center program manager to make the system change.
- Results: Now, they successfully use tenecteplase and have updated protocols, stroke education, and order sets. Not enough eligible patients have received tenecteplase to see an improvement in door-to-needle time yet, but this is a great start.
Award Qualifications
- Impressive teamwork to remake current stroke education, orders, and workflows that affected multiple departments.
- Cooperation and creativity for a successful rollout.
Hudson Hospital & Clinic and Lakeview Hospital,
Acute Stroke Ready Hospitals
Stillwater, Minnesota; Hudson, Wisconsin

- Opportunity for Improvement: Improve door-to-treatment times for their catchment areas.
- Action Plan: Using Lean tools, the team learned that each step before receiving thrombolytic treatment had factors lengthening the time to treatment. The team learned that there was a large need for stroke education, which had been a struggle to keep up with during the COVID-19 surges. They created different kinds of staff education materials to reach all learning styles.
- Results: There have not been any treatment cases to measure an improvement in door-to-needle time. However, other measures of success include improved recognition of stroke symptoms, decreased door-to-imaging time, and more staff engagement.
Award Qualifications
- Pooled resources at many sites within a health system and led a partnership to impact a large service area.
- Thoughtful and broad approach to improving time measures during a challenging time and fewer patients than usual.
2022 Outstanding Achievement Award Recipients
This is an award for an initiative that led to evidence-based positive change in the quality of stroke care.
Essentia Health St. Joseph's Medical Center,
Primary Stroke Center
Brainerd, Minnesota
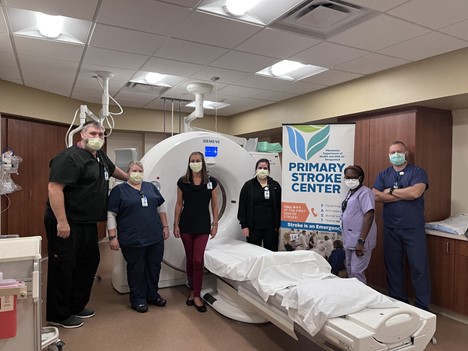
- Opportunity for Improvement: Improve door-to-CT times for those arriving by private car.
- Action Plan: The department team shared stroke alert data and developed a new process. They updated the private car stroke alert process so the patient would go straight to the CT when stroke activation criteria were met. The team improved times through teamwork, quickly recognizing stroke symptoms, and activating the stroke alert for patients in private cars, the same way patients arriving by EMS would.
- Results: Since beginning the project, there has been an improvement in times and the team met the goal in Q2 of 2022.
Award Qualifications
- Addressed a difference in care quality among their patients who arrived by EMS versus private car.
- Led to future projects to address more equitable stroke care in the community served.
Regions Hospital,
Comprehensive Stroke Center
St. Paul, Minnesota

- Opportunity for Improvement: Meet the new goal for at least 50% of eligible patients receiving endovascular treatment within 90 minutes of arrival through better decision-making.
- Action Plan: The team reviewed the current workflow. They assessed different time metrics from when the patient came to the emergency department to when the device is placed in the endovascular. They learned that phone calls were causing extra delays. The team gathered the endovascular therapy team at the hospital. Based on their ideas, Regions began a secure text messaging application with high-quality image sharing to quickly alert the team and reduce phone calls.
- Results: Multiple time metrics have improved since the application has been used. The team met and went above the goal of the 50% threshold since the project went live.
Award Qualifications
- Examined the many steps in stroke care for patients that could be adding to delays.
- Looked for creative approaches to the issue.
