Asthma
- Asthma Home
- About Asthma
- Minnesota Asthma Alliance
- Managing Asthma
- Data
- Training Resources
- For Schools
- For Health Care Professionals
- For Homes
- For Communities
- For Workplaces
- Who We Are
- COVID-19 and Asthma
- Enhanced Asthma Care Services Act
Resources
- Asthma Education Resources for American Indian Communities
- Asthma Home-Based Services
- Asthma Home-Based Services Toolkit, Manual and Client Curriculum
- Engaging the Latine Community Around Asthma
- Outdoor Air Quality Guidance for Schools and Child Care
- Strategic Framework
Related Sites
Asthma
- Asthma Home
- About Asthma
- Minnesota Asthma Alliance
- Managing Asthma
- Data
- Training Resources
- For Schools
- For Health Care Professionals
- For Homes
- For Communities
- For Workplaces
- Who We Are
- COVID-19 and Asthma
- Enhanced Asthma Care Services Act
Resources
- Asthma Education Resources for American Indian Communities
- Asthma Home-Based Services
- Asthma Home-Based Services Toolkit, Manual and Client Curriculum
- Engaging the Latine Community Around Asthma
- Outdoor Air Quality Guidance for Schools and Child Care
- Strategic Framework
Related Sites
Asthma Home-Based Services
On this page:
Impact of offering asthma home visits in Minnesota
Get started
Toolkit, Manual, and Client Curriculum
Make a referral
The Minnesota Asthma Program encourages local public health, Tribal health and other health-based agencies to incorporate Asthma Home-Based Services (AHBS) into their routine home visiting programs.
Home-based services are a unique opportunity for a health care professional to visit the individual with asthma in their own home. Meeting with individuals and families at their home creates the opportunity to provide the following:
- Personalized asthma self-management education support (includes medication and asthma action plan reviews).
- Assessment of the home environment to identify and support trigger mitigation.
It is important that individuals with asthma understand and know their asthma triggers. What may cause their asthma symptoms and learn ways to reduce exposure or eliminate triggers as much as possible. What may trigger a person’s asthma is very specific to that individual.
Home-based services afford more time with the individual and give the health care professional an opportunity to assess the home for potential asthma triggers. Health care professionals can use the results of the environmental home assessment to understand trigger exposure and better tailor a plan to support daily asthma self-management.
Impact of offering asthma home visits in Minnesota
Asthma home visiting services are an evidence-based method for improving health outcomes, lowering healthcare utilization costs, improving patient care, and reducing health disparities; yet far too many people with poorly controlled asthma don’t have access to these key interventions.
In Minnesota, provision of asthma home visits and durable medical equipment (e.g. mattress encasements, vacuum cleaners, and HEPA filters) to children with asthma has the potential to avert over 60,000 symptomatic days and save Minnesota over $1M annually through reduced ER visits.
Minnesota spotlight
Minnesota is featured as one of the success stories from across the country in the Sustainable Financing For Home-Based Asthma Services: Snapshots of Innovation and Progress Across the Country. The report highlights both state Medicaid policy advances, and stories about local partnerships, pilot programs, and other innovations that create a groundswell for statewide change; all serving as models for new community action.
Get started
A referral, coming from the individual's prescribing health care provider, school nurse, public health nurse or community health worker is the first step in getting an asthma home visit scheduled for a individual with uncontrolled asthma.
Health care systems, clinics, and providers struggle with sufficient time to provide asthma education in the clinic setting and they do not have the opportunity to see what triggers maybe affecting their patient's asthma in the patient home.
Home visits can provide asthma care that meets the medical and educational needs of the individual. Medical treatment, including daily medications, in addition to effective management of asthma environmental triggers in the home can reduce the number and severity of an individual's asthma episodes.
Toolkit, manual, and client curriculum
Asthma Home-Based Services Toolkit provides resources and educational tools to support local public health or other health-based organizations interested in developing asthma home-based service programs. Peer-to-peer mentoring is available by pairing experienced local public health staff with agencies that are interested in providing asthma home-based services in their community.
Make a referral
The following Minnesota programs currently offer in-home services for asthma. Please see contact information to inquire about services provided and current eligibility.
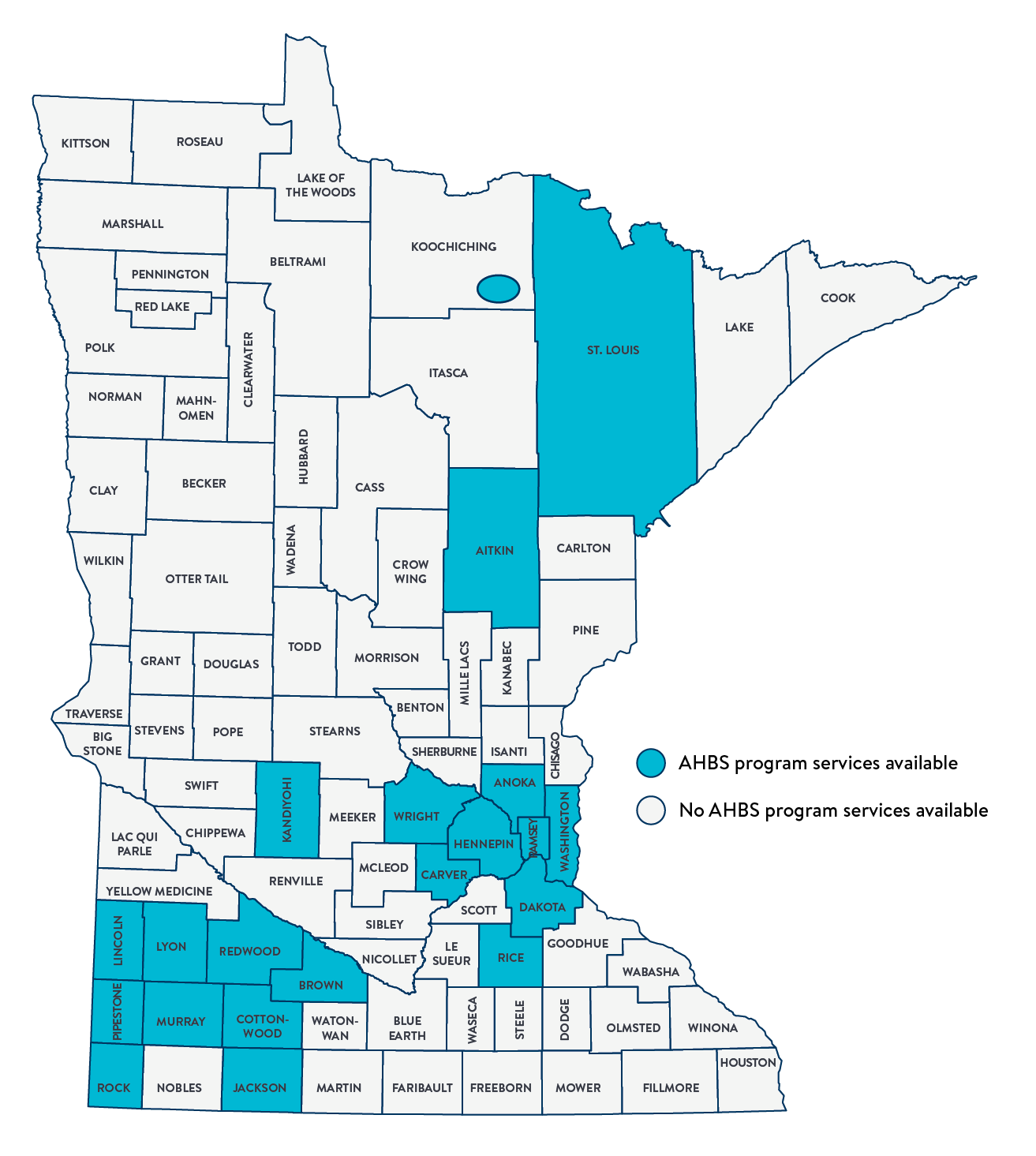
Map information
Agencies offering asthma home-based services to counties they serve: Aitkin, Anoka, Brown, Carver, Dakota, Des Moines Valley Public Health, Hennepin County, Kandiyohi County Health and Human Services, City of Minneapolis, Ramsey County, Southwest Health and Human Services, Rice County, St. Louis County Public Health, and Wright County.
Services include free asthma consults for children that reside in that county. Services include an in-home asthma visit by a public health nurse or asthma program health care team member.
All other counties: are not offering Asthma Home-Based Services currently.
Aitkin County Public Health seeks to support all children with asthma, who are 17 and younger, and live in Aitkin County by offering free in-home asthma services.
A public health nurse with specialized training in asthma management can help in the following ways:
- Conduct in-home assessments to identify asthma triggers.
- Provide recommendations for trigger reduction and offer supportive equipment when appropriate.
- Provide asthma self-management education, including action plans and medications guidance.
- Offer care coordination and support.
Contact Aitkin County Public Health:
- Call 218-927-7200. Ask to speak with Naomi
- Email public-health@aitkincountymn.gov
Anoka County offers free asthma consultations for children up to age 18 who live in Anoka County and have an asthma diagnosis.
A public health nurse can visit clients in their home up to three times to:
- Provide education on current asthma action plan.
- Provide education on medication use.
- Provide an asthma home assessment to look for asthma triggers.
- Connect to community resources.
Submit a referral by one of the following:
- Visit Anoka County Asthma Program.
- Complete the online submission form at Anoka Public Health Nursing Referral.
- Call our Public Health Nurse Intake Line at 763-324-4240 and complete a referral over the phone.
Email: Public.Health.Nursing@anokacountymn.gov
Brochures:
Asthma Brochure - English (PDF)
Asthma Brochure - Spanish (PDF)
Brown County offers free asthma consultations for children up to age 18 who live in Brown County and have an asthma diagnosis. A public health nurse can visit clients in their home up to three times to:
- Provide an asthma home assessment.
- Identify asthma triggers to improve asthma control and reduce asthma symptoms.
- Provide individualized asthma self-management education.
- Connect to community resources.
For more information or to sign up:
- Visit our website Asthma Program | Brown County, MN
- Call our office at 507-233-6820
- To make a referral visit Brown County Public Health - Asthma Home Based Services Program
Contact email: Melissa.Hoffmann@broncountymn.gov
Flyers:
Carver County Public Health offers free asthma consultations for children age 17 and younger who live in Carver County and have an asthma diagnosis. A public health nurse will partner with your family to help reduce your child’s symptoms.
Home visits may include:
- Understanding asthma and common home triggers
- Identifying ways to reduce your child’s symptoms
- Reviewing or helping develop an asthma action plan
- Connecting your family with helpful community resources
Contact Carver County Public Health:
- Visit: Carver County Public Health Asthma Program
- Make a referral: Public Health Nursing Referral: Home Visit for Child with Asthma
- Call: 952-361-1329
- Email: public-health@carvercountymn.gov
Dakota County offers free asthma consultations for children ages 17 and younger who live in the Dakota County and have an asthma diagnosis.
A public health nurse can visit and work with the family on ways to reduce the child’s symptoms. The nurse can help the family learn about asthma, discuss community resources available to decrease exposure to triggers in the home, and assist in developing an asthma action plan.
Contact Dakota County Public Health:
- Visit: Dakota County Public Health Asthma Consultations.
- Call: 651-554-6115.
- Email: PHintake@co.dakota.mn.us.
Des Moines Valley Public Health is dedicated to supporting children ages 0 to 18 with asthma who live in Cottonwood or Jackson counties.
Our asthma home-visiting program can provide free in-home visits provided by a public health nurse with special education in asthma management.
A home visit allows more time with children and their caregiver (s) to learn more about asthma and self-management, discover and mitigate potential asthma triggers, and receive guidance on how to use asthma medications and maintain an asthma action plan. To schedule a visit, call Des Moines Valley Public Health or email asthma@dvhhs.org.
Contact Des Moines Valley Public Health:
- Visit: Des Monies Valley Health and Human Services.
- Call: 507-831-1987. Ask to speak with Genna or Erin.
- Email: asthma@dvhhs.org.
Hennepin County will provide asthma home visits for eligible county residents, including families who live in Minneapolis.
A public health nurse specializing in pediatric asthma will:
- Educate regarding asthma diagnosis and what it means for the child and the child’s family.
- Provide asthma self-management education; understanding the different roles of medication and devices.
- Conduct home environmental assessment for asthma triggers and make referrals for possible home remediation or other resources.
- Reinforce and educate regarding the child's asthma action plan.
- Coordinate clinic and provider appointments to ensure continuity of care.
Contact Hennepin County Public Health:
- Email: familyhv@hennepin.us.
- Web: hennepin.us/homevisiting.
- Phone: 612-348-TOTS (612-348-8687), Option 1.
- Complete Home visiting referral online form.
Contact City of Bloomington – Public Health Department: (If you reside in Bloomington, Richfield, or Edina contact Bloomington Public Health below):
- Email: publichealth@bloomingtonmn.gov
- Web: https://www.bloomingtonmn.gov/ph/public-health
- Phone: 952-563-8900
- Complete Public Health Services Referral form
Kandiyohi offers free asthma home visits for all individuals (children and adults) who live in Kandiyohi County and have poorly controlled asthma or are newly diagnosed. A trained public health nurse will:
- Educate about asthma and provide asthma self-management education.
- Conduct home environmental assessment for potential asthma triggers and education about how to reduce identified triggers.
- Provide area resource information, coordination, and support.
- Educate and provide individual instruction on how to use asthma medications.
- Assistance with developing an asthma action plan.
- Individuals may be eligible to receive free trigger-reducing products.
Contact Kandiyohi County Public Health at 320-231-7800, Select Option 4, or email at publichealth@kcmn.us.
Minneapolis Asthma Program offers asthma home visits for Minneapolis residents with children under 21 years of age diagnosed with asthma. The Minneapolis Health Department will provide the following:
- A trained specialist to conduct a free walk-through of your home to find common asthma triggers and discuss ways to reduce or remove asthma triggers. Includes up to three visits from a public health nurse - more visits may be added if necessary.
- Free allergen-reducing products, such as a HEPA air purifier, furnace filter, HEPA filter vacuum, and dehumidifier to improve the indoor air quality.
- Free allergen pillow and mattress covers.
- Free professional pest control.
Contact the Minneapolis Health Department at 612-673-2301, or text 612-449-0778, or email at health@minneapolismn.gov.
For additional information: City of Minneapolis Asthma Program.
The Healthy Homes program offers a free 1-hour visit with an environmental health specialist and a public health nurse to assess homes for asthma triggers and to provide asthma self-management education. The goal of this program is to help families reduce environmental triggers of asthma and to create a healthier home environment for their children.
Ramsey County residents with children under 18 years old who are diagnosed with asthma, may be eligible to receive free products to help manage their children's asthma. Some of these products may include a HEPA air cleaner, HEPA vacuum, bed and pillow encasements, cleaning supplies, radon test kit, and pest control supplies.
A home assessment includes:
- An opportunity to discuss your child's asthma action plan or asthma symptoms with a registered nurse.
- An opportunity to learn how your home environment may be impacting your child's health.
Contact Ramsey County Healthy Homes Program at HealthyHomes@ramseycounty.us or call 651-266-1199 to schedule an asthma home visit.
For additional information: Ramsey County Healthy Homes Program.
Rice County offers free asthma consultations for children 0-18 who live in Rice County and have been diagnosed with asthma.
Rice County’s asthma home-based services are a unique opportunity for a public health nurse to meet with you and your child in your own home. The public health nurse can provide the following:
- Individualized education
- Review asthma action plans
- Assess the home environment
- Suggest equipment to help manage asthma and answer questions in a comfortable environment for both child and caregivers. Families may be eligible to receive free trigger-reducing equipment.
Information flyers:
Contact Rice County Public Health by visiting their Public Health Online Referral Form
Call: 507-332-6111
Email: rcpublichealth@ricecountymn.gov
Southwest Health & Human Services (SWHHS) is a multicounty agency offering free asthma home consultations for children ages 0-17 years who have asthma and live in one of the following counties: Lincoln, Lyon, Murray, Pipestone, Redwood, or Rock.
A SWHHS public health nurse that specializes in asthma management can visit and work with the family on ways to reduce the child's symptoms. These visits can help the family learn about asthma, discuss community resources available to decrease exposure to triggers in the home, and assist in developing an asthma action plan.
Contact Southwest Health and Human Services:
- Visit: Asthma Home-Based Services - Southwest Health and Human Services.
- Call: 888-837-6713.
- Email: asthma@swmhhs.gov.
St. Louis County offers free asthma home visits for children (0-18) living in St. Louis County who have poorly controlled asthma. A St. Louis County public health nurse can:
- Conduct a home assessment for asthma triggers.
- Provide asthma self-management education.
- Offer care coordination and support.
- Provide one-on-one instruction on how to use asthma medications and on the importance of following an individualized asthma action plan.
- Tools and equipment may be available to help reduce asthma triggers in the home.
Contacts for St. Louis County:
- North St. Louis County contact: Sarah Wipf, public health nurse, at 218-471-7608 or wipfs@stlouiscountymn.gov (Hibbing, Virginia, Ely and surrounding areas).
- South St. Louis County contact: Kelly Bruels, public health nurse, at 218-725-5212 or bruelsk@stlouiscountymn.gov (Duluth, Proctor, Hermantown, Saginaw and surrounding areas).
For additional information: St. Louis County Asthma Home Visiting Program.
Wright County offers free asthma consultations for children 0-17 or through high school who live in Wright County and have been diagnosed with asthma.
Wright County's asthma home-based services are a unique opportunity for a public health nurse to meet with you and your child in your own home. The nurse can provide individualized education, review asthma action plans, assess home environment, suggest equipment to help manage asthma, and answer questions in a comfortable environment for both child and caregivers. Families may be eligible to receive free trigger-reducing equipment.
Contact Wright County Public Health:
- Visit: Wright County Environmental Health.
- Call/text: 763-335-0280.
- Email: H.S.PublicHealth@co.wright.mn.us.
